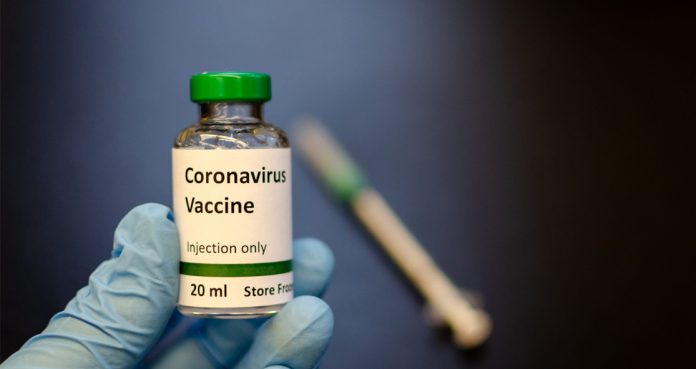
Moderna Therapeutics, a Cambridge, Massachusetts-based biotechnology company, has shipped the first lots of its coronavirus vaccine to the National Institute of Allergy and Infectious Diseases (NIAID). The vaccine will be ready for human trials in April.
NIAID is a part of the National Institutes of Health (NIH) in Bethesda, Maryland.
Moderna created the vaccine in just 42 days after Chinese researchers released that the genetic sequence of the coronavirus (COVID-19) is similar to SARS-COV-2. The company focuses on discovering and developing drugs and vaccines based on messenger-RNA (mRNA).
NIH researchers also began testing an antiviral drug called remdesivir, which is developed by Gilead Sciences. The drug had been developed for treating Ebola.
Remdesivir is undergoing human trials for treating COVID-19 at the University of Nebraska Medical Center. The first patient who volunteered for the study is a passenger who was repatriated from the Diamond Princess cruise ship. Gilead’s antiviral drug showed promising results in pre-clinical studies.
Volunteers will receive either remdesivir or a placebo intravenously for 10 days. The study researchers will analyze their blood tests and nose/throat swabs every two days to measure the amount of virus in their bodies. The drug could help contain the spread of the virus even if it shows some efficacy in keeping the viral load from rising.
The new COVID-19 vaccine developed by Moderna is based on a new genetic method, which is packed with mRNA, a genetic material that comes from DNA and makes proteins.
The vaccine is loaded with mRNA that codes for the coronavirus proteins, which is then injected into the body. The generic material is then processed by the immune cells in the lymph nodes to make the protein for other immune cells, recognizing and marking them for destruction.
President of Moderna Dr. Stephen Hoge told TIME, “mRNA is really like a software molecule in biology. So our vaccine is like the software program to the body, which then goes and makes the [viral] proteins that can generate an immune response.” That means this new vaccine method could be scaled up quickly, which will save critical time when new diseases, such as COVID-19, emerge and start infecting a large number of population.