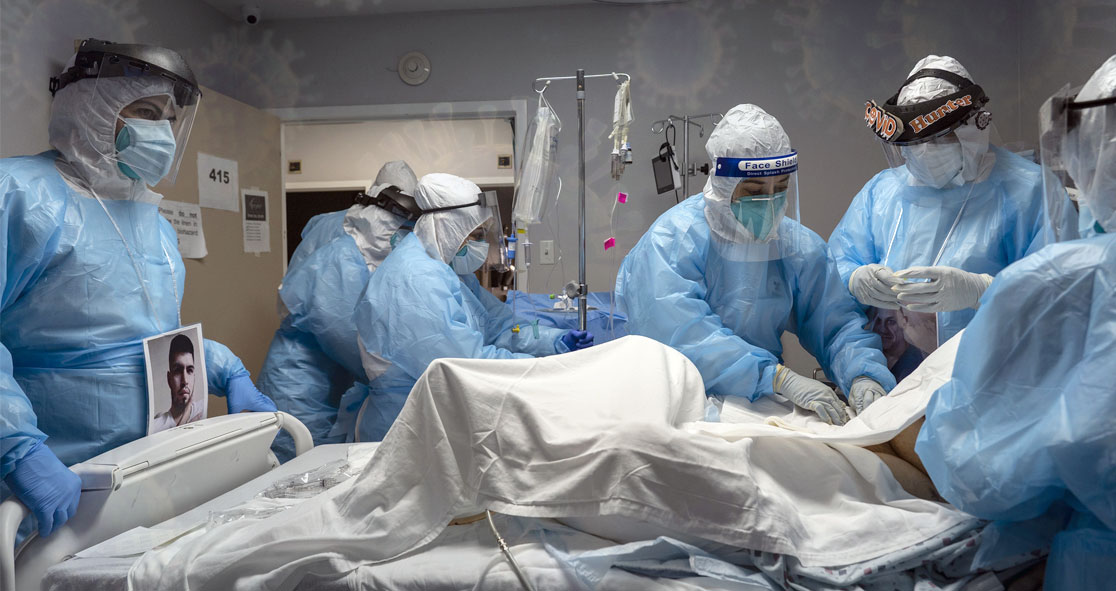
A new study has found that at least 8 in 10 patients hospitalized with COVID-19 infection develop neurologic complications, and they are more likely to die in hospital than those without neurologic complications.
The study, published online Tuesday in JAMA Network Open, revealed that 82% of hospitalized COVID-10 patients had neurological implications, with a six-fold increased death risk.
Principal investigator Dr. Sherry Chou told Medscape Medical News, “We now know that neurological conditions are common in hospitalized patients with COVID-19, and in this large study we can see the impact of neurological conditions.”
“Without really knowing whether the neurological conditions directly cause these patients to die,” she added, “we do see that patients who have neurological conditions with COVID-19 were more likely to die while they’re in the hospital/”
Dr. Chou is an associate professor of critical care medicine, neurology, and neurosurgery at the University of Pittsburgh School of Medicine, Pennsylvania.
She noted, “The challenge to us as physicians and scientists is to figure out why and how we can prevent that.”
The study looked at more than 3700 patients hospitalized with COVID-19 and found that over 82% developed neurological manifestations. Most patients reported neurologic symptoms such as headaches, anosmia (loss of smell), and ageusia (loss of taste).
Among all those patients, acute encephalopathy, coma, and stroke were the most common neurologic signs or syndromes.
The researchers also found that these neurological signs or syndrome were associated with an increased risk of death during hospitalization.
Dr. Chou explained, “Having a preexisting neurological condition of any kind most reliably and most strongly predicted the development of COVID-19-related neurological complications. The risk is more than double compared to those who don’t have a preexisting neurological condition.”
“For patients hospitalized with COVID-19 who develop neurological problems, it may take a very long time to recover,” she added. “Many of these patients continue to deal with these symptoms and disabilities long after they have beat COVID.”
“Even if the pandemic is completely eradicated, we are still talking about millions of survivors who need our help,” Dr. Chou continued. “It is important to find out what symptoms and health problems those patients are facing, and there is still plenty of work for years to come.” The article was published on Medscape Medical News.