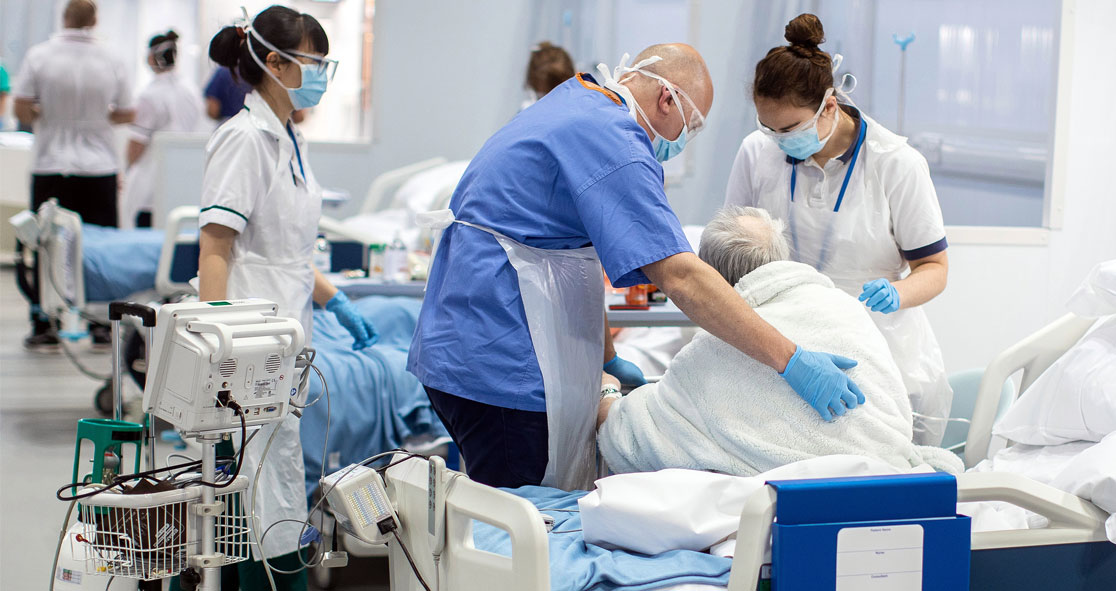
According to a leaked NHS document, Greater Manchester will be running out of beds to treat seriously ill COVID-19 patients, while some of the hospitals in the region are already full.
Last Friday, the resurgence of the virus had left hospitals in Stockport, Salford, and Bolton with no spare beds due to the growing influx of the patients.
The current scenario prompted ministers to make a deal with local leaders about Great Manchester’s planned move to the top-level (Tier 3) of COVID-19 restrictions.
The NHS’s leaked document suggested that the city’s hospitals are quickly running out of beds for people with coronavirus who need emergency care to save their lives.
As of Friday, in Greater Manchester, more than 80% of the total supply of critical care beds were already being used.
The revelation came as the current political impasse continued between the government and Andy Burnham, the mayor of Greater Manchester, other local leaders, and MPs.
Under Tier 4 lockdown restrictions, ministers require Greater Manchester to follow the toughest sort of local lockdown. However, Burnham said this “can only happen with greater support for businesses forced to close such as pubs, and those left without income,” according to the Guardian.
On Sunday, Michael Gove, Minister for the Cabinet Office, escalated the government’s war of words with Burnham by accusing him of risking lives by opting for “press conferences and posturing” instead of agreeing to new COVID-19 rules.
Many doctors raised concerns over the rapidly worsening situation in Greater Manchester.
Consultants Committee Chair of British Medical Association Dr. Rob Harwood said, “These projections paint a stark picture, with the possibility in a worst-case scenario that some intensive care units in the city potentially run out of beds within weeks. They also suggest that the number of patient deaths may even overtake those seen during the peak of the pandemic earlier this year.”
“The last thing we want to see is a repeat of the numbers of cases – and the subsequent pressures on hospitals – that we saw back in April,” he continued, “but worryingly this analysis forecasts just that.”
“The situation in the region is alarming, with the number of new infections remaining worryingly high, and doctors are incredibly concerned that unless the rate of transmission is curbed urgently, it is possible that we may soon see a further increase in patients needing intensive care and, tragically, an increase in deaths,” Dr. Harwood added.
Meanwhile, a spokesperson for the NHS in Greater Manchester said, “We are monitoring the situation with our hospital admissions, overall beds, and ICU beds very, very closely.”
“It’s not unusual for 80-85% of ICU beds to be in use at this time of year and our hospitals work together if there are particular pressures in any one area, to ensure the best care for patients who need the high level of support ICU provides, both for COVID and for other reasons,” the spokesperson added.
A renowned NHS expert in Liverpool said, “There have been a number of ICU patient transfers over this weekend to try to cope with demand. Staff absence levels are running a bit more than double normal sickness rates. There is very little ‘spare’ ICU capacity in the region.”
NHS officials in Greater Manchester have been considering opening the city’s Nightingale hospital in the next few weeks to meet the fast-growing influx of COVID-19 patients. However, it is unclear where the staff needed will come from, as the other hospitals are already jam-packed.
Dr. Nick Scriven of the Society for Acute Medicine said that finding the staff to work in them could pose a challenge. “The big question for the Nightingales is how will they be staffed,” Dr. Scriven said. “Given the pressures on all ICU wards, how can they release their staff to other units if the intention is to look after level two or three patients there? There needs to be some very clear guidance and thought put into who the Nightingales will be tasked with looking after.”