A clinical trial by the University of Cincinnati added an immunotherapy drug to standard treatment and found that it increased survival rates for head and neck cancer patients with intermediate-risk features, according to Science Daily.
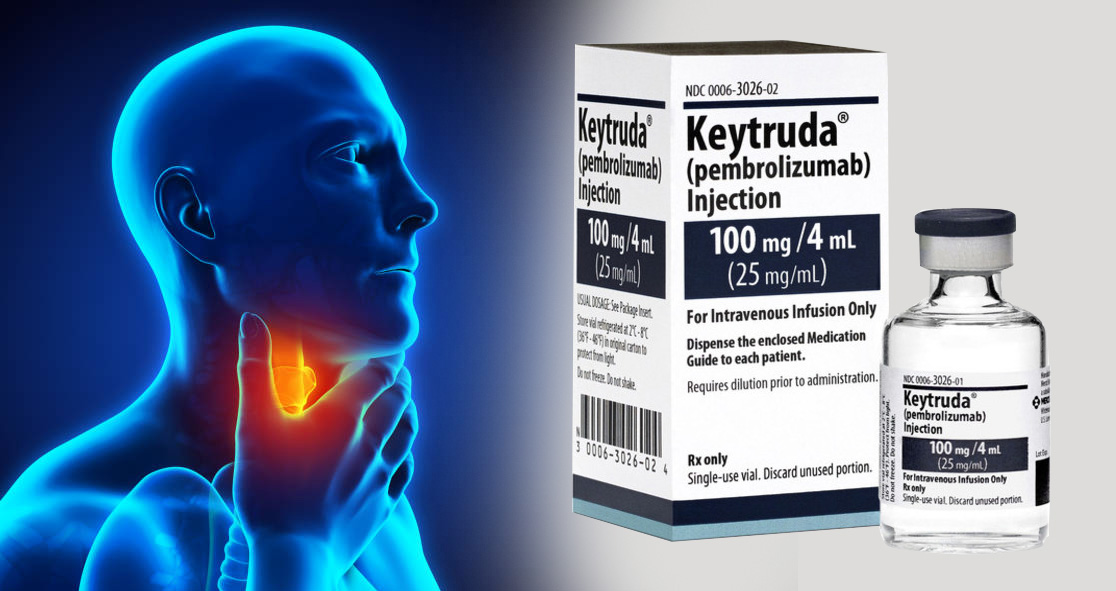
Lead author Dr. Trisha Wise-Draper said the trial focused on adding a drug, pembrolizumab (Keytruda), to patients’ typical standard care of treatments.
Keytruda is an antibody used in cancer immunotherapy that treats various cancers, including head and neck, Hodgkin lymphoma, stomach cancer, cervical cancer, and certain types of breast cancer. It blocks PD-1 located on lymphocytes. This receptor prevents the immune system from attacking the body’s own tissues – the so-called immune checkpoint.
Dr. Wise-Draper explained, “Once the virus or infection is cleared, you have to have a way to turn your own immune system off, to tell it that the infection is gone and it’s time to calm down.”
She said pembrolizumab has been developed as a treatment for multiple cancers and it has shown early success as a treatment for head and neck cancers that have spread or returned after initial treatment. Previous studies reported that the drug is 20% effective.
“And although we’re careful to say cure, it does result in what is called ‘durable responses,’” Dr. Wise-Draper explained, which means patients have a good response to treatment much longer than expected, sometimes for years, “which was a huge advancement over chemotherapy where they may have only been effective for say nine to 10 months at most.”
The study, published in the journal of the American Association for Cancer Research, found that Keytruda caused the death of tumors before surgery in nearly 50% of patients.
Dr. Wise-Draper said, “We could see that a lot of these tumors were dying even after that first dose of pembrolizumab. That was pretty exciting because that was higher than we expected.”
More than 95% of patients in the study reported one-year disease-free survival when treated with both pembrolizumab and radiation.
Dr. Wise-Draper said, “We had a huge improvement in that, so we saw that pembrolizumab was definitely increasing their chance of survival, at least compared to historical controls.”
In addition, in patients where pembrolizumab began to kill the tumor before surgery, 100% reported one-year disease-free survival.
She said, “It was a really strong predictor of patients who are going to do well on this treatment. Hopefully that is going to help us design trials to better understand who is going to respond and who is not.”
Researchers at Harvard University have conducted a similar trial that showed similar success. The successful findings of these trials show that a Phase III clinical trial is worth pursuing.
In fact, Merck is in the process of conducting a randomized clinical trial comparing patients who receive pembrolizumab along with the standard of care versus patients who receive the standard of care only.
Dr. Wise-Draper said of the Merck trial, “That will be a much larger study that will help show if pembrolizumab truly benefits these groups.”
She added, “It’s been extremely exciting to see patients do well on this study and seeing their survival increase knowing what the historical rates were, as well as just being able to have a successful study in general is pretty exciting. A lot of these developments I didn’t expect to happen so quickly in my career, so it’s really been an exciting process for all of us. Hopefully there’s more to come.”
She also said that if pembrolizumab continues to prove safe and effective, it would mark a “huge improvement” compared to the current standard of care that can still lead to a 50% recurrence rate.
“There is even a possibility that patients would not need their treatment plan to include surgery” Dr. Wise-Draper added. “If we have a treatment that is less toxic, maybe we can cut down on the morbidity of surgery and radiation as well as the chemotherapy.”