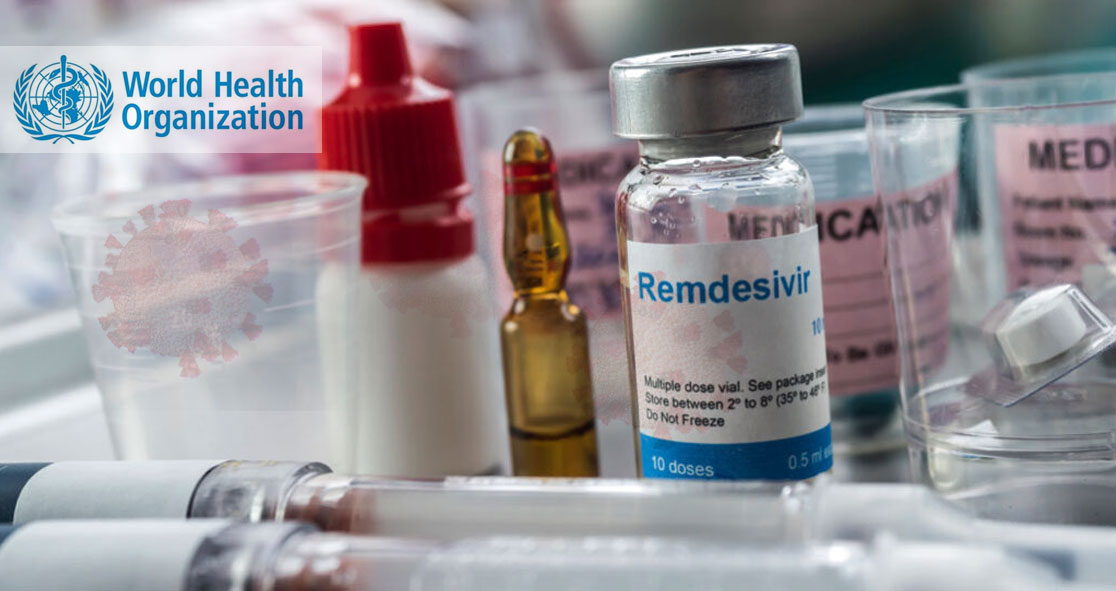
A study funded by the World Health Organization (WHO) found that remdesivir is ineffective at reducing hospitalized COVID-19 mortality.
The study also found that the drug does not even shorten the recovery time of patients who do survive, contradicting the findings of previous smaller studies that found remdesivir, an antiviral drug developed by Gilead Sciences, helped hospitalized COVID-19 patients recover faster.
Those previous studies prompted the FDA to announce Emergency Use Authorization (EUA) for remdesivir. Thousands of COVID-19 patients have received the drug in the United States, including President Donald Trump.
The WHO-funded study was conducted between March 22 and October 4, involving 11,330 patients from more than 400 hospitals in 30 countries. The patients received either remdesivir alone or a combination of remdesivir and three other drugs.
The study authors said, “These remdesivir, hydroxychloroquine, lopinavir and interferon regimens appeared to have little or no effect on hospitalized COVID-19, as indicated by overall mortality, initiation of ventilation and duration of hospital stay.”
The findings of the study were released online in the preprint server medRxi. It has not been peer-reviewed or published in any scientific journal yet.
Gilead issued a statement defending its antiviral drug, adding that controlled studies “published in peer-reviewed journals validated its benefits.”
The company also raised questions about how the WHO-sponsored study was conducted, stating there was variation in “trial adoption, implementation, controls and patient populations and consequently, it is unclear if any conclusive findings can be drawn from the study results.”
Infectious disease expert Dr. Peter Chin-Hong of the University of California, San Francisco, told The New York Times that large studies in different countries could result in inconsistent treatment methods. He said, “So much goes into care. The drug is only part of it.”
Gilead originally developed remdesivir for the treatment of Ebola, which was repurposed to treat COVID-19.
Dr. Julie Fischer of Georgetown University said of the study, “It’s certainly disappointing. What all of us would like to see is what is frequently called a ‘magic bullet’; a drug that’s already in existence, that is safe and works effectively in patients.”
“Unfortunately, in this case, this trial at least suggests the benefits of remdesivir weren’t there at all,” she added.
The FDA granted EUA to remdesivir in April, stating, “While there is limited information known about the safety and effectiveness of using remdesivir to treat people in the hospital with COVID-19, the investigational drug was shown in a clinical trial to shorten the time to recovery in some patients.”
A clinical trial conducted by the National Institutes of Health (NIH) found remdesivir effective at shortening recovery time in more than 30% of patients. The NIH said the trial “suggested a survival benefit, with a mortality rate of 8.0% for the group receiving remdesivir versus 11.6% for the placebo group.”
However, the WHO-funded study said remdesivir and the other drugs just did not work. The study researchers said, “The unpromising overall findings from the regimens tested suffice to refute early hopes, based on smaller or non-randomized studies, that any will substantially reduce inpatient mortality, initiation of ventilation or hospitalization duration.”