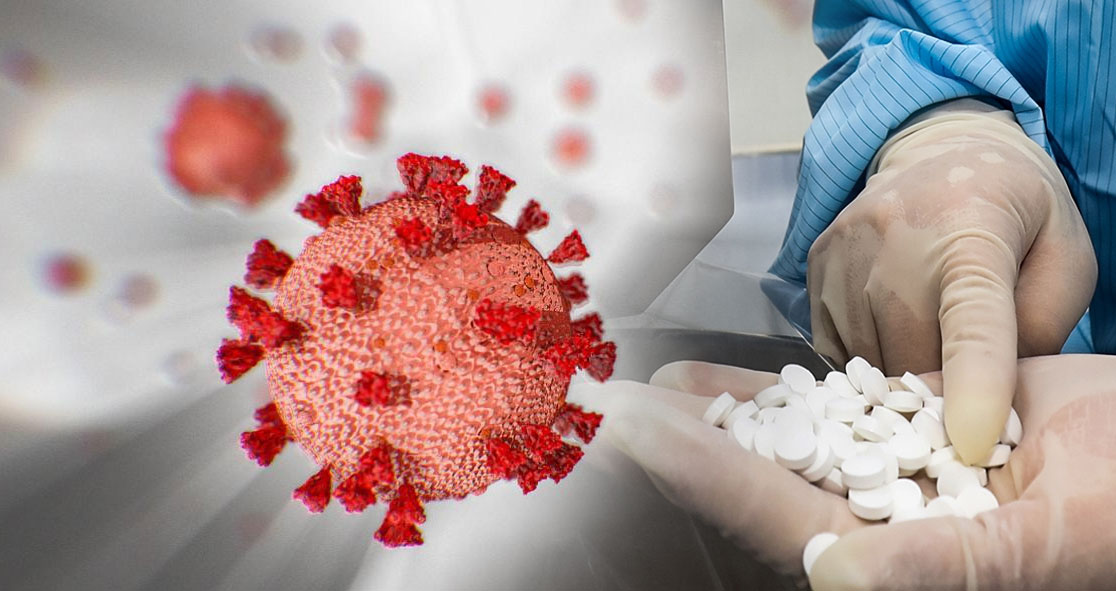
A biologist at the University of Virginia (UVA) is in the hope of developing a drug cocktail to treat COVID-19.
In 2014, Dr. Judith White, Professor of Cell Biology at UVA, and her team began working on a drug cocktail to treat Ebola. Similarly, they figured that using this concept of drug cocktails could help treat COVID-19.
She explained, “With HIV and hepatitis C virus, there are anywhere between two and four drugs. The basic concept is to hit the virus at different sites in the viral life cycle.”
“It minimizes the chance of getting drug-resistant mutants, and the other thing is you can lower the doses,” she added.
The team used a strategic approach by combining several drugs based on certain factors.
Dr. White said, “It’s basically how potent they are at blocking the virus in cell culture. What are the levels of the drug over time in your bloodstream, in the lung. How quickly does it decay, which would impact how frequently you have to take the drug as well as what’s known about how the virus replicates.”
Unfortunately, their Ebola drug cocktail research was slowed by a lack of funding.
The enthusiasm for this approach waned as the risk of Ebola fell. However, since the COVID-19 arrived, Dr. White and her colleagues started working on models that can help craft different drug cocktails for each viral family.
Dr. White said, “There are 11 families of human viruses that are considered of pathogenic potential. If a new virus is suspected, we would know very quickly: Is it a coronavirus? Is it a filovirus? Is it a flavivirus? We would have on-the-shelf drug cocktails A, B, C, D, E so to speak, and we would know if it’s a flavivirus, cocktail C has a really good chance of working on it. The idea is to make these cocktails against the whole virus family.”
She explained that generic drugs, which have already been approved, could be combined to treat new diseases.
“They’re very inexpensive, and they are room temperature stable,” the UVA biologist noted. “They don’t need to be frozen. They’re oral drugs, so it has much more global potential. They could be used in low- and middle-income countries. They could be easily shipped over there.”
“You don’t need specialized, skilled clinical people to administer them, so we think of them as practical and thoughtful drug combinations for the whole world,” she added.
Dr. White also explained that for each virus family, testing must be done on the right kind of cells.
She said, “One issue with COVID, in particular, is when you do the work in the cells, you have to do it in a lung cell. A lot of the early work has been done in a cell line that’s not really relevant to COVID disease, notably hydroxychloroquine, ivermectin. They don’t work in lung cells, and so they were really non-starters.”
Dr. White and her team hope their approach will help the world to get prepared for future pandemics.
She said, “The idea in terms of pandemic preparation is to really just tamp down the infection within an individual and within the population at the very earliest time after we know that something is brewing.” She said, in the meantime, the best way to overcome the pandemic is to get vaccinated.